Cannabis advocates are typically quick to tout the plant as a medical marvel, which can provide unprecedented relief from all kinds of conditions, including migraines, which affect more than 36 million people in America alone.
But how much do we really know about the herb which has been ever-present throughout recorded human history, but kept prohibited for much of the past century?
The short answer: more than ever.
Now for the long answer.
Before diving deeper into the medicinal potential of cannabis products for migraines, it’s important to have a base knowledge of the cannabinoids in the plant, and an understanding of how these interact with the body – specifically, with the endocannabinoid system (ECS), as many cannabis researchers believe that dysfunction in this network could be the root cause of migraines.
An introduction to CBD and THC, the most important cannabinoids in cannabis
There are no fewer than 113 cannabinoids in cannabis, most of which we still know very little about. This alone suggests that it will be decades before we understand the full implications that cannabis has on the body, and how it can best be used to treat illness.
However, scientists have explored the plant’s two most-abundant cannabinoids – cannabidiol (CBD) and delta-9-tetrahydrocannabinol (THC) – in some depth. The key difference between them is that THC is psychoactive while CBD is not, but both have distinct medicinal qualities which may aid the treatment of migraines.
THC is a partial agonist of the CB1 and CB2 receptors. The former is found mostly in the central nervous system, and are implicated in multiple variables, including pain perception, appetite and mood. The latter is predominantly in the peripheral nervous system, and mostly influences immune system response. THC is the cannabis plant’s version of anandamide, an important endocannabinoid and neurotransmitter which helps to maintain the ECS. Therefore, taking THC can help to compensate a deficiency of anandamide.
THC = nutrient for our endocannabinoid receptors
“Currently, however, statistically significant differences in cerebrospinal fluid anandamide levels have been documented in migraineurs.”

In contrast, CBD is an antagonist of these receptors, and therefore has a much different therapeutic effect. Rather than binding to receptors and working as an endocannabinoid substitute, CBD affects the ECS so that concentrations of anandamide and 2-AG, another endocannabinoid, are increased. Anandamide is degraded by fatty acid amide hydrolase (FAAH), a catabolic enzyme, but CBD can interfere with this process. CBD = potency increaser of endocannabinoid substitutes How it manages this remains somewhat unclear: a study on mice showed CBD to be an FAAH inhibitor, although research published in the peer-reviewed Journal of Biological Chemistry in 2015 found a different effect in humans. This study found that CBD “inhibits the cellular uptake and catabolism of anandamide” by binding with fatty acid-binding proteins (FABPs), which are responsible for transporting anandamide to FAAH enzymes. In the coming years, medical scientists will surely find out much more about the subtle interactions of cannabinoids, but it is increasingly apparent that cannabinoids play a vital role in regulating the ECS, and that they can also treat imbalance in the system.
Why migraines aren’t just headaches
Migraines and headaches are often mistaken for being one and the same, but there are some key differences to be aware of. Headaches are a broad range of pains in the head region of which migraine is a subset of. Headaches are shorter and generally less painful but there are exceptions for clusters, thunderclaps etc. Migraines, however, cause intense pain at the front or side of the head, which can persist for days. Other symptoms, which migraineurs refer to as an “aura”, are often a pre-warning of when a migraine is about to strike. These are the result of neurological changes, and could be any of the following:
- Physiological symptoms: fainting, tingling, spinning sensation, weakness
- Auditory symptoms: increased sound sensitivity, speech and hearing disturbances
- Psychological symptoms: mood and appetite changes, memory issues, loss of control
- Visual symptoms: flashing lights, stars, wavy lines and general increased light sensitivity
The psychological symptoms, in particular, are an indication that migraines have an adverse effect on the ECS.
Migraine patients need new solutions
The encouraging research behind cannabis for migraines is not just welcome, but as a necessity. Many patients find that current drugs, both over-the-counter (OTC) and prescription, either do not provide sufficient relief, or cause side effects. Triptans, such as Axert and Flova, are meant to reduce symptoms by influencing serotonin receptors – serotonin is a hormone associated with happiness and general wellbeing. But some patients have reported chest and throat tightness, sleepiness and tingling when taking these drugs. A study recently conducted in Italy compared the effectiveness of a cannabinoid treatment comprised of CBD and THC with amitriptyline, a tricyclic antidepressant drug used to treat migraines, in addition to depression and anxiety. The first phase of the research involved just the cannabinoid concoction, which was given to 48 participants who suffered from chronic migraines.
The treatment was given in an oral dose of 200mg and was found to reduce acute pain symptoms by 55 percent.
This is likely the effect of the cannabinoids on the CB1 receptor, which can be influenced to reduce the body’s sensitivity to pain. The second part of the study pitted the CBD and THC treatment against the amitriptyline – 79 patients were administered either 200mg of the former or 25mg of the latter over three months. Meanwhile, a further 48 patients with cluster headaches were treated with the same THC-CBD dose, or 480mg of verapamil, a calcium channel blocker. The results found medical cannabis to be slightly more effective than the amitriptyline, and that the only notable side effects were reduced concentration and drowsiness, while reducing pain intensity by 43.5 percent. Fascinatingly, while the CBD-THC mix only abetted some of the cluster headaches, the treatment was particularly successful at managing pain in those who had suffered from migraines since an early age. Ideally, a follow-up study would look more closely at why cannabis worked for those patients but did not treat acute symptoms in those with no long-term history of migraines. Leader of the research, Dr Maria Nicolodi, said of the study, “We were able to demonstrate that cannabinoids are an alternative to established treatments in migraine prevention.” Prior to cannabis prohibition, the herb was a very popular treatment for migraines in both Europe and North America between 1842 and 1942, according to Western pharmacopoeias. While this may seem surprising given today’s perception of cannabis, given its proliferation as a medicine for migraines and other illnesses in the ancient civilizations of China, Egypt, Greece and elsewhere, we perhaps shouldn’t be shocked. See the graph below for the favourite aspects of CBD products reported by users in 2017 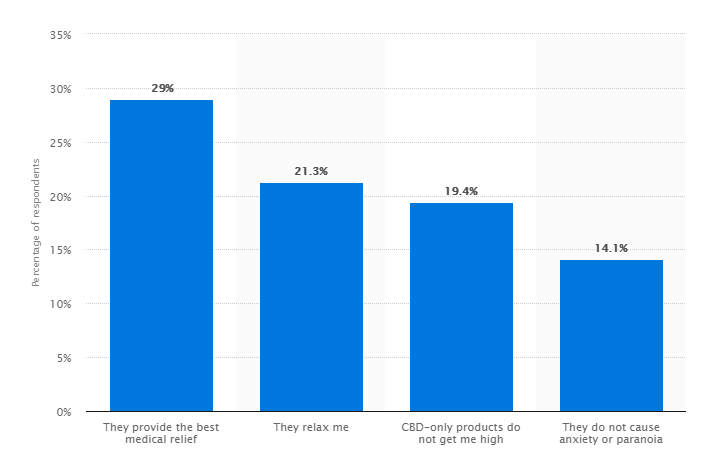
What is Clinical Endocannabinoid Deficiency?
Clinical Endocannabinoid Deficiency (CECD) is a medical concept which may explain why cannabinoids are an effective medicine for various conditions– the bulk of research on this theory concerns irritable bowel syndrome (IBS), fibromyalgia and migraines. CECD was first proposed by neurologist and psychopharmacology researcher, Dr Ethan Russo, in December 2003. Follow-up papers have expanded on the concept, although legal barriers to the study of medicinal cannabis has inevitably stifled progress. However, those studying CECD have made a series of intriguing discoveries on the relationship between migraines and the endocannabinoid and serotonin systems. Anandamide has been shown to potentiate the 5-HT1A receptor and inhibit the 5-HT2A receptor. Research has revealed that the heightened light and sound sensitivity experienced by migraine patients is perhaps due to an overactive sensory hyperalgesia, which the ECS may correct via interactions within the central nervous system. Many scientists have linked migraines to the trigeminovascular system. Interestingly, studies have shown that endocannabinoids have an effect on this system, further supporting the idea that the ECS is key for the treatment of migraines. Research on trigeminovascular neuronal responses indicates that migraines and cluster headaches may be relieved with a CB1 receptor agonist, although the study’s authors expressed doubt over the use of psychoactive substances such as THC. An Italian study found that rates of anandamide hydrolysis, or breakdown, were higher in the platelets of migraine sufferers – it’s possible that the reduced serum anandamide levels mean that these patients have a lower pain threshold and are therefore more vulnerable to intense migraines. Another study investigating CECD looked at anandamide concentrations in the cerebrospinal fluid (CSF) of migraineurs. The researchers determined that the reduced anandamide levels in chronic migraine patients supported the concept of ECS failure being at the root of the condition. This could be due to anandamide not fulfilling its role as a modulator of the trigeminovascular system.
“A study presented at the Congress of the European Academy of Neurology in Amsterdam confirmed that cannabinoids are just as suitable as a prophylaxis for migraine attacks as other pharmaceutical treatments.”
There is a lack of focused trials on the usage of THC and other cannabinoids in the treatment of migraines – most currently available information relates to surveys and case reports of medicinal marijuana use. However, a recently released Colorado study of migraineurs (more than two-thirds of whom had a history of cannabis consumption) showed cannabis to reduce headache frequency by more than half, from 10.4 to 4.6 attacks per month. Unfortunately, the exact cannabinoid profile of the strains used is unknown but were likely to be high in THC.

CBD as a standalone treatment for migraines
Many migraineurs are keen to know whether CBD can work as a standalone treatment, or if a whole-plant treatment, which features psychoactive THC, is also necessary. Frustratingly, despite having immense therapeutic value, THC can be disabling in the
See our video on CBD and migraines below:
Which products may offer relief from migraines?
The cannabis industry has evolved, and both medicinal and recreational users have a variety of products to choose from, all of which provide unique forms of relief. In the past, cannabis was typically used either by smoking it or by eating a cannabis-infused edible. There are plenty of health risks from smoking, but the fast onset of effect of cannabinoids when inhaled can be very useful at treating acute pain symptoms. This rapid relief explains why vaporizing has become such a popular method of consumption. CBD vape oil and e-liquid is sold in multiple flavors and potencies. Understandably, taking medicine by smoking or vaping it is not for everybody. Even though a 2015 report from Public Health England determined vaping to be 95 percent safer than smoking, the risk to the lungs is not totally negligible – for smokers trying to quit, vaping is a great choice, but for non-smokers, perhaps not so much. In this case, CBD oil is the next best option for quickly blunting migraine pain. This is administered under the tongue with a pipette or dropper, and held for two to three minutes, while the CBD is sublingually absorbed into the bloodstream through the tissues in the bottom of the mouth. For a migraine that has persisted for several hours or even days, CBD edibles, capsules and any CBD product that is ingested may be effective. These can be advantageous over sublingual oils and e-liquids, in that the CBD remains active in the ECS for up to six to eight hours, meaning the patient doesn’t have to top up their medication as often. The downside is that edibles do not work as quickly – the cannabinoids only become active after being absorbed through the stomach, which can take an hour or more. Therefore, CBD edibles are not recommended for acute pain relief. CBD topical products are mostly used for improving skin conditions by reducing inflammation or for cosmetic purposes, such as anti-aging. However, CBD massage gels and creams are also popular for relieving localized pain. Since the pain from migraines is concentrated at the front and side of the head, CBD topicals may have a therapeutic effect, perhaps by interacting with the vanilloid (TRPV-1) receptor, which is expressed in the skin.  The hemp-based CBD industry is also split into two types of products: isolated CBD and full-spectrum CBD. CBD is the only cannabis constituent in CBD-isolate products, while full-spectrum products are made with a full hemp extract. The presence of other non-psychoactive cannabinoids – and there are more than 100 of these, only a few of which have been properly researched – looks to boost the therapeutic value of the CBD. This reaction between the cannabinoids and terpenes in a full-extract is synergistic and known as the “entourage effect”.
The hemp-based CBD industry is also split into two types of products: isolated CBD and full-spectrum CBD. CBD is the only cannabis constituent in CBD-isolate products, while full-spectrum products are made with a full hemp extract. The presence of other non-psychoactive cannabinoids – and there are more than 100 of these, only a few of which have been properly researched – looks to boost the therapeutic value of the CBD. This reaction between the cannabinoids and terpenes in a full-extract is synergistic and known as the “entourage effect”.
The legal prospects for cannabis-based medication
All this talk about the medicinal possibilities of cannabis for migraines is great, but without legislation that widens access to these products, migraineurs will be left stranded. Thankfully, hemp-derived CBD products are legal pretty much everywhere and have become widespread in the United States and throughout Europe, as consumers sample the cannabis that “doesn’t get you high.” The second decade of the 21st century has been a very positive one for cannabis. As of 2018, cannabis is recreationally legal in nine US
What does this all mean?
The research available presents a clear link between migraines and irregularities in the endocannabinoid system – this indicates that cannabis can treat this peculiar
“Migraine headache frequency decreased from 10.4 to 4.6 headaches per month with the use of medical marijuana”
At present, it seems as if CBD products are effective at treating migraines – and these also provide several other benefits to physical and mental health through regulation of the ECS. However, the full potential of cannabis for migraines may not be unlocked unless THC is also part of the medication. For patients unable to access THC treatment, the best solution looks to be full-spectrum CBD. As these products are made with a whole-plant extract, the patient can receive some benefits of the “entourage effect”. Furthermore, a full-spectrum product in the United States can contain up to 0.3 percent THC, which will give an additional, yet non-intoxicating therapeutic effect. CBD is often compared with medications like
